This story is one of many exploring recent advances in the science of longevity and aging. The following few articles in the series, including this one, will focus on the relationship between genetics and longevity; Which genes are involved in aging and longevity? How are they involved? What are the therapeutic implications?
Aging is the biggest risk factor for Parkinson’s disease, a disorder of the central nervous system that causes uncontrollable movements and shaking. Although treatments are available, there is currently no cure; we can help manage symptoms, but we don’t yet know how to tackle the root causes. A new study may offer clues. Published in Molecular Psychiatry, the research uncovers a previously unidentified genetic mutation that provides a significant protective effect against Parkinson’s disease. Understanding the mutation might open new avenues for treatment and prevention.
The “Forgotten” Genome: Mitochondrial DNA
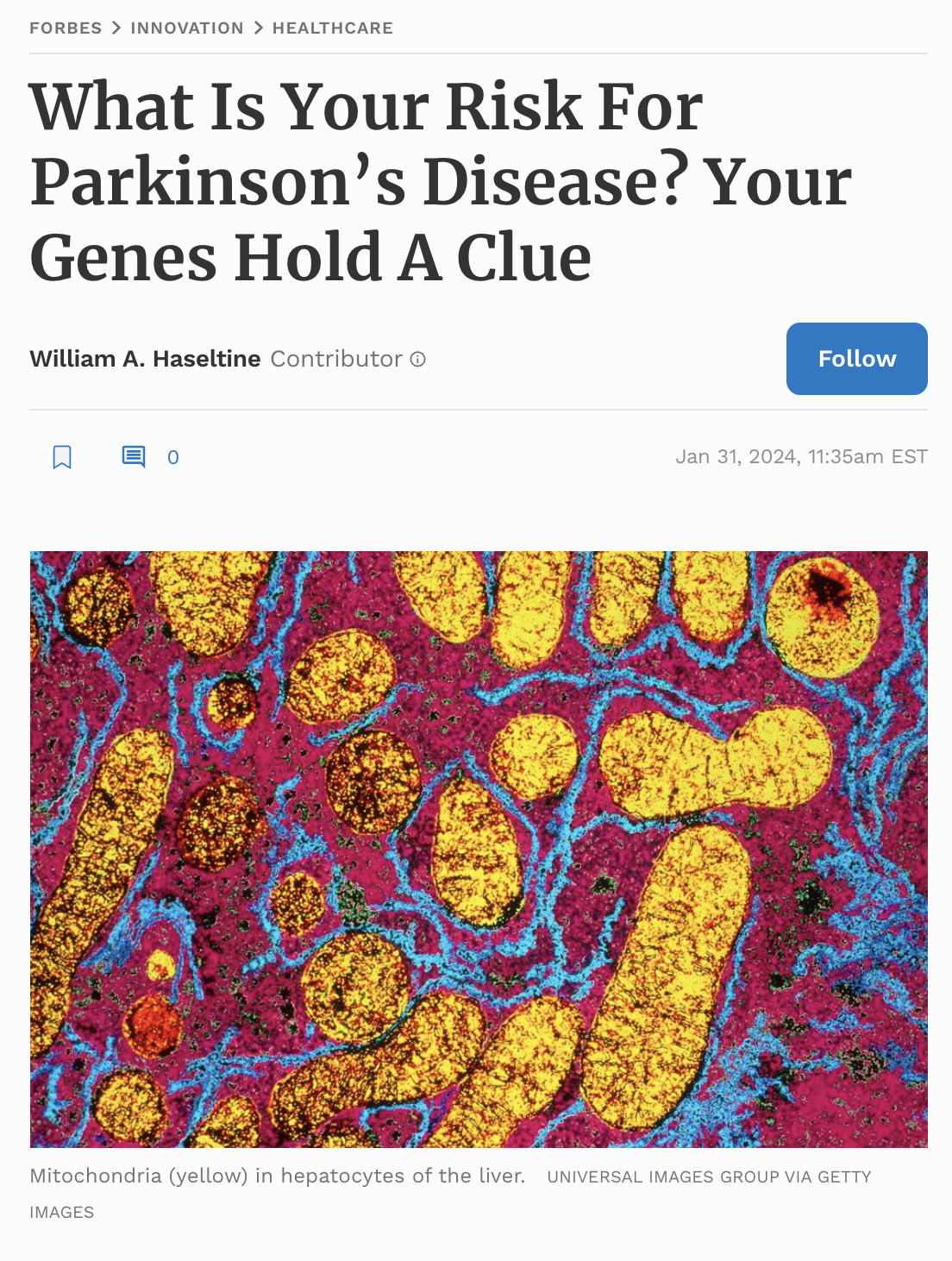
When you think of genes, you probably think of DNA (deoxyribonucleic acid), the iconic molecule that carries our genetic code. Now, most DNA is housed in the nucleus of cells, which acts both as a safe room for our genetic material as well as a cellular control center of sorts. But a small portion of our DNA —roughly 1%— is housed elsewhere: the mitochondria. The name may ring a bell. These special organelles, many will recall, are the powerhouses of the cell. They help convert energy from food into a cell-friendly format, enabling all kinds of important functions.
Mitochondrial DNA (mtDNA) is different from the run-of-the-mill DNA found in the nucleus. For one, the mitochondrial genome is circular rather than linear. It is also markedly smaller, clocking in at roughly 16,500 base pairs compared to the almost 3.3 billion base pairs found in the nuclear genome. And where a large portion of nuclear DNA is “noncoding”, meaning it does not carry any proteins, the majority of the mitochondrial genome does encode proteins.
One such mitochondrial protein is called small humanin‐like peptide 2 (SHLP2). It was first discovered in 2016 by the Pinchas Cohen Laboratory at the USC Leonard Davis School. Follow-up experiments showed that the micro-protein helps protect against age-related diseases like cancer. Also, the levels of the protein fluctuate in those who suffer from Parkinson’s disease. After an initial spike, likely in an attempt to minimize the damage caused by the disease, production quickly slows and eventually flatlines
Genetic Variant Is Extra Protective
In this latest study, researchers with the Pinchas Cohen Laboratory returned to the protein to see if they could find anything new. They assembled data from thousands of human study subjects gathered as part of the Health & Retirement Study, Cardiovascular Health Study, and Framingham Heart Study. They then screened the mitochondrial DNA of these subjects to check for any variation in the gene that produces small humanin-like peptide 2.
Indeed, they noticed that around 1% of the population —primarily those of European ancestry— carried a point mutation, meaning a single change to one of the letters that make up the gene. On the surface, this may seem like a tiny difference, but it has serious implications: carriers of the variant are 50% less likely than the rest of the population to develop Parkinson’s disease.
The newly identified mutation alters the structure of the protein, making it more stable and leading to a higher rate of expression. This increased stability, in turn, helps the protein curb mitochondrial dysfunction, which is a key factor in the development of Parkinson’s disease.
How? The researchers noticed that small humanin-like peptide 2 is present in the mitochondria of neurons, which are the fundamental cells of our central nervous system, responsible for sending and receiving sensory information across the body and the brain. In particular, the microprotein binds to an enzyme called mitochondrial complex 1. This enzyme, which helps kickstart the production of cellular energy, is a critical regulator of metabolism; deficiencies in mitochondrial complex 1 have been associated with Parkinson’s disease, heart attacks, and strokes.
The protective variant of small humanin-like peptide 2 binds the enzyme especially tightly, delaying the decline of the enzyme’s activity. So, those with the variant have improved mitochondrial complex 1 function, and by extension, fewer issues with mitochondrial dysfunction.
Takeaways
Parkinson’s disease is one of many age-related health conditions. As with others, it reduces quality of life and life expectancy. This new study by researchers at the University of Southern California helps highlight several important points. First, it pinpoints a previously unknown protective genetic variant found in mitochondrial DNA — carriers of which enjoy a twofold reduction in risk. In doing so, it serves as a powerful reminder that the mitochondrial genome, all too often overlooked or sidelined, may play an influential role in a number of age-associated diseases. Second, the study provides a detailed description of the molecular mechanism by which this mutation helps protect its carriers. Down the road, we may be able to use this newfound information to develop effective therapeutic interventions that mimic the beneficial effects of the gene.