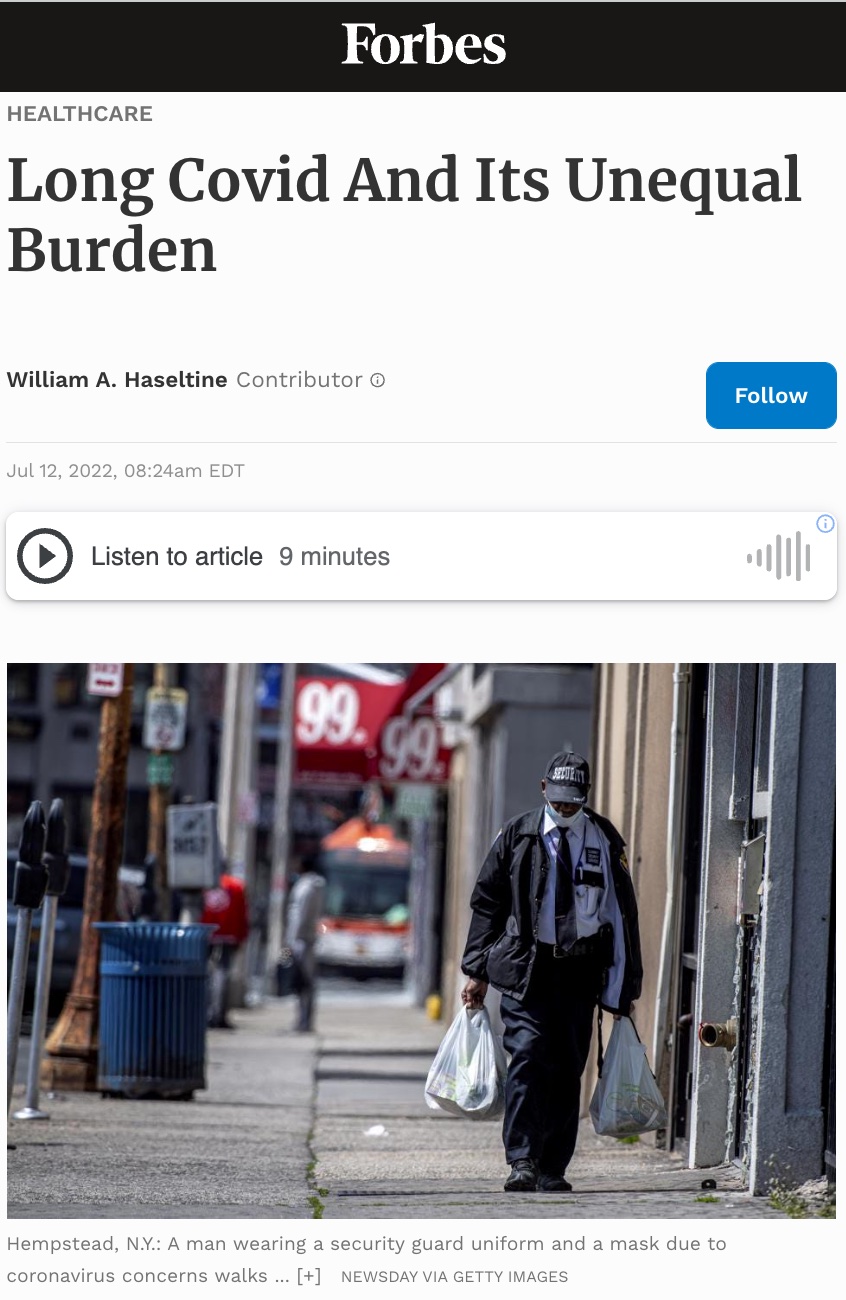
All countries have health disparities, or unfair and avoidable differences in health status between groups. As defined by WHO, these differences come “from the social conditions in which people are born, grow, live, work and age,” factors which extend beyond an individual’s control. The United States is no exception. The beginning of the Covid-19 pandemic provided a clear example of how health disparities exist for certain racial and ethnic groups in the US.
Black, Latino and American Indian persons experienced higher rates of Covid-19 infection, hospitalization and death than white, non-hispanic persons. Genetic predisposition to health conditions like lung disease and hypertension contribute to these numbers, but greater still are the societal factors which influence these statistics. Marginalized groups are more likely to live and work in crowded settings and to have less income and wealth. As a result these groups were, and still are, more likely to catch Covid-19 than others, but are less equipped to face the economic strain which accompanies testing, treatment and recovery.
The current state of the pandemic, now two and a half years in progress, has left at least 20 million people Covid survivors in the US facing post-Covid Conditions—otherwise known as Long Covid. And while it is uncertain whether people of diverse backgrounds have higher genetic risk of developing the condition, communities of color will likely face exacerbated effects of Long Covid as a consequence of persisting health inequities. In particular, the heightened probability of infection, reduced access to primary/specialized care, and diminished economic position faced by minority populations will translate to a more arduous road to Long Covid recovery.
Heightened probability of infection
Long Covid can develop from asymptomatic, mild and severe acute Covid-19. There currently is no cure-all for the condition; treatment is offered based on the displayed symptoms and any traceable organ damage. Correspondingly, the best method to avoid Long Covid at present is to prevent getting Covid-19 to begin with. In this regard, racial and ethnic minorities are at greater risk of SARS-CoV-2 infection than others due to work and living conditions.
As explained in the paper Long Covid and Health Inequities: The Role of Primary Care, people of color are overrepresented in high risk and essential occupations. Healthcare workers, transport workers, and members of the service industry come in contact with large quantities of people but have less ability to physically distance themselves. Adequate proper personal protective equipment (PPE) may not be given. These factors increase the chances of contracting Covid-19 and subsequently Long Covid.
The environment at home also contributes to the likelihood of acquiring Covid-19. The high-density areas and crowded homes occupied disproportionately by vulnerable groups make it easier to spread Covid-19 and harder to isolate. Evidently, racial and ethnic groups face obstructions even at this first line of defense.
Reduced access to primary/specialized care
Once post Covid complications emerge, the critical next steps are to diagnose and treat symptoms and/or organ damage. A primary care physician (PCP) familiar with a patient’s health history would be more equipped to notice the unusual symptoms of Long Covid and refer the individual to specialized services, such as a multidisciplinary Long Covid clinic. Although this process proves difficult for most people with Long Covid and similar chronic conditions, people of color face additional barriers which aggravate access to treatment.
A 2020 poll by the African American Research Collection found Black, Native and Latino Americans reported having less access to a primary care doctor than their white counterparts.
A possible contributor is geographic constraints. A disproportionate number of Black and minority ethnic groups live in medically underserved areas which lack access to primary care. Even if primary care is available, inadequate public transportation can delay medical care.
Access to care is further complicated by perceived levels of discrimination and medical mistrust—all which racial and ethnic minorities experience disproportionately.
Location impacts specialist care, as well. Several US states only have one multidisciplinary Long Covid clinic, if at all. Essential workers will have a harder time requesting time off work and traveling to necessary appointments. Dr. Monica Lypson states it best in this STAT article: “People who were putting our groceries on the shelves, people in the transportation industry like Metro or bus drivers — the idea that you’d be on the phone trying to find a clinic that potentially was an hour to four hours away from you is a lot.”
Coupled with geographic constraints is health insurance access. People of color are more likely to lack health insurance, as many jobs held by non-white groups do not provide sufficient healthcare benefits. This is especially true for Latinos. Recent results from the NCHS Household Pulse Survey estimate up to 17% of Hispanics or Latinos are currently uninsured. This is compared to 12% of people of multiple races, 10.6% of Black Americans, and 7% of white Americans. Considering that Long Covid symptoms often take months to resolve, the ability to pay for continued treatment will disadvantage minorities preferentially.
Diminished economic position
All stages of Long Covid diagnosis and treatment are intrinsically impacted by one’s economic means. People with Long Covid must cover the costs for doctor’s visits, medication, therapy, and transportation. The most common symptoms of Long Covid—fatigue, post-exertional malaise, brain fog and shortness of breath—often force people to leave work, suspending one’s income stream (at least temporarily). Money, therefore, is a major deciding factor in Long Covid recovery.
Many racial and ethnic groups are less likely to possess the financial cushion needed to support those with Long Covid. As previously mentioned, minorities are overly represented in frontline, essential work. These positions earn less and are often inflexible to schedule changes. Temporary leave for recovery may not be an option. For some, it is better to suffer at home than risk losing their jobs or endangering household income by seeking treatment.
Trevon Logan and Bradley Hardy explore how economic inequalities create disproportionate health burdens on Black Americans in their essay, Racial Economic Inequality Amid the COVID-19 Crisis. Logan and Hardy emphasize how Black Americans face higher income volatility, higher unemployment, and greater levels of food and housing insecurity than many other Americans. These factors left Black Americans more vulnerable to acute Covid-19 crises; similarly, the lack of economic buffers for Black families will translate to worse Long Covid outcomes for this minority.
Future Considerations
Topics of health inequity and Long Covid still require investigation. Some studies such as UCSF Clinical trial on Long Covid are striving to increase minority representation in their Long Covid research, but for now, much of what is known is based on research with stronger representation from higher income, predominantly white cohorts. Despite this fact, one can expect disadvantaged groups to bear a heavier burden caused by Long Covid by inferring known associations between race/ethnicity, health disparities, and acute Covid-19.
The pandemic is far from over—vaccines do not yet protect against infection, and statistics on new cases and hospitalizations are rising with the spread of Omicron variants BA.5 and BA.275. The population of Americans experiencing Long Covid symptoms will likely continue to grow. Now more than ever will the country need health policies which lessen cost barriers to care, improve insurance coverage, and bolster primary care systems. A stronger foundation in equitable health policy will not only help our disadvantaged communities weather the current Covid-19 storm, but also prepare the country for any possible future pandemics.