
This story is part of a series on the current progression in Regenerative Medicine. This piece discusses advances in brain-machine interfaces.
In 1999, I defined regenerative medicine as the collection of interventions that restore to normal function tissues and organs that have been damaged by disease, injured by trauma, or worn by time. I include a full spectrum of chemical, gene, and protein-based medicines, cell-based therapies, and biomechanical interventions that achieve that goal.
In the United States alone, roughly two million people are living with limb loss, the majority of whom deal with prosthetic limbs daily. Often cumbersome and imprecise, traditional prosthetic limbs are challenging to use effectively and fall well short of the functionality of the original limb. Even more advanced robotic limbs are still far from perfect.
Among the best artificial limbs are those outfitted with an electromyography (EMG) sensor, which monitors incoming movements from remaining muscle groups and translates that data to the appropriate motion in the prosthetic. However, these sensors tend to be bulky and sensitive to perspiration and pressure.
A recent study in NPJ Flexible Electronics by Dr. Jaeu Park and colleagues from Daegu Gyeongbuk Institute of Science & Technology in Korea outlines a flexible and durable EMG sensor designed as a thin dermal surface, overcoming the shortcomings of previous EMG devices.
Here, I will discuss their sensor and its future in regenerative medicine.
Akin to many of the smart fabrics I have discussed over the past several months in this series on regenerative medicine, Park’s dermal surface EMG is fashioned in two layers. The first layer is a silicon base, which creates structural integrity for the electronics. The second layer consists of overlaid electrodes that can activate and transmit data to an external destination; all encased in insulation to prevent discomfort for the wearer. The collective is less than half a millimeter or less than the tip of a sharpened pencil.
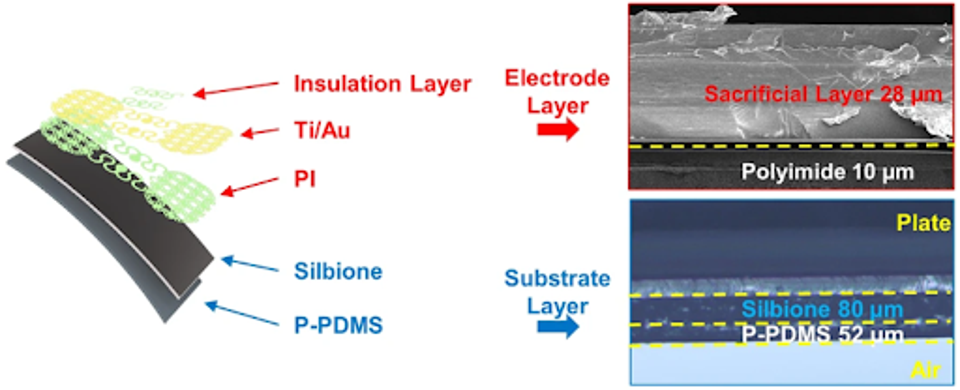
FIGURE 1: Specific description of the electrode layer and base layer of the sEMG sensor.
Fitted along the calf or quadriceps, based on the area of amputation of the patient involved, the sensor monitors muscle contracts. These contractions are monitored and quantified from patient to patient, then mapped based on how the muscle contracts during specific walking motions.
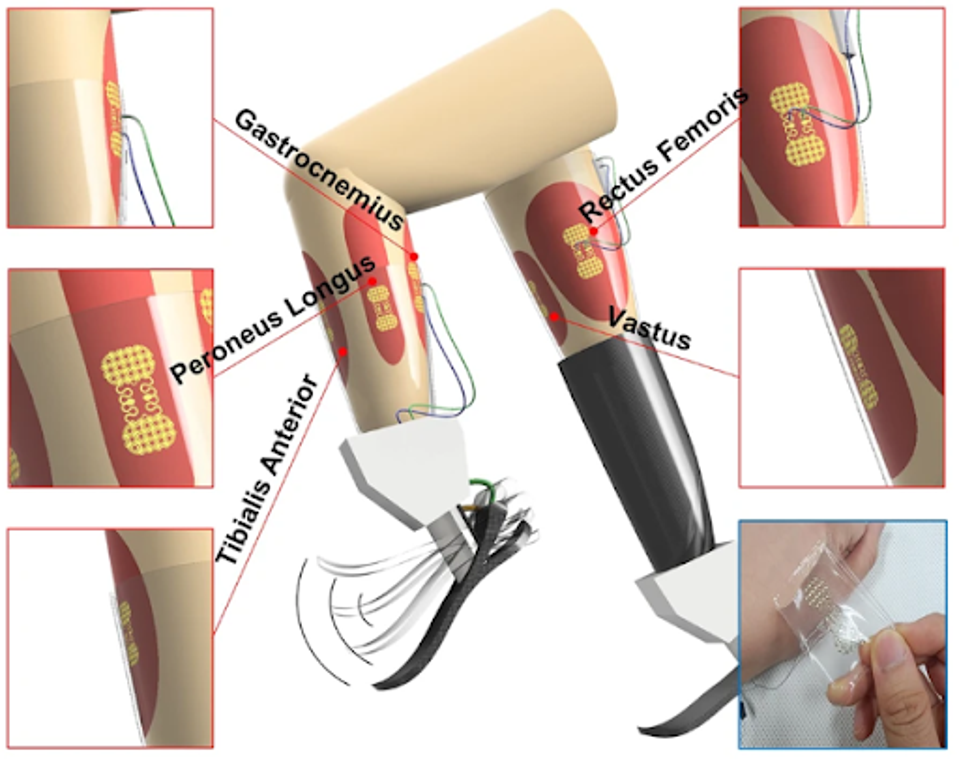
FIGURE 2: sEMG sensor attached to different types of muscles in the legs.
With sufficient mapping data, the electrodes in the sensor can capture muscle movement and transmit that data to a processor in the prosthetic, which activates a motor, completing the motion. In theory, this would allow the user to walk normally without special consideration for the prosthetic or any cumbersome electronic accessories.
With a cohort of three lower limb amputees, the system worked well to monitor muscle movement and effectively translate data to prosthetic response. Notably, the system adapted well to varying stages of amputation, with the three patients being amputees between three and 25 years. The three-year amputee had trouble isolating individual muscle flexion during the learning stages, while the other two had fewer issues. Still, the EMG system effectively adapted to the patient, maintaining incoming reception of muscle movement.
Further, there are a number of applications for the EMG system outside of the prosthetic enhancement. Some that come to mind include rehabilitation, such as monitoring and evaluating muscle activity and progression in stroke patients, for instance. Another use may be for diagnostics to monitor those at risk for degenerative muscle or bone disease to preempt regression.
The system is fascinating but still in its infancy. As with all emerging regenerative techniques I analyze, there is always room for continued research, development, and enhancement. A primary concern I typically have with brain-machine style innovations is the cost. However, in most instances, I expect the robotic prosthetic to outweigh the cost of the EMG sensor material.
My main concern for Park and company’s EMG is continued research to ensure viability, but this system is well on its way to improving the lives of many in the years to come.
To read more of this series, please visit www.williamhaseltine.com


