This story is part of a series on the current progression in Regenerative Medicine. This piece discusses advances in the use of artificial intelligence in medical robotics.
In 1999, I defined regenerative medicine as the collection of interventions that restore to normal function tissues and organs that have been damaged by disease, injured by trauma, or worn by time. I include a full spectrum of chemical, gene, and protein-based medicines, cell-based therapies, and biomechanical interventions that achieve that goal.
As robotics and artificial intelligence technologies advance, their combined use in medicine will become pronounced as time marches on. Both robotics and artificial intelligence are widely used in the medical field today. Robotics are used in surgery to assist doctors in delicate procedures, robotic exoskeletons are used in rehabilitation from injury or illness, and so on. Artificial intelligence is used to assess diagnoses and treatment plans, as well as accelerating medical research and drug development.
How, then, can these technologies be combined to improve medical practices and health outcomes? In a perspective for Science, Dr. Michael Yip and colleagues discuss the present and future of artificial intelligence and medical robots. Here I will summarize and comment on their findings.
The first region of medicine Yip and colleagues query with respect to artificial intelligence medical robots is image guidance and surgery. While robots may have been used previously to assist in image capturing, for example, when detecting lesions or other malicious tissues, human assistance was always required to recognize the tissue and diagnose.
Artificial intelligence presents the opportunity to both drive robots during biopsies to detect dangerous masses as well as create diagnoses for what the masses may be. Artificial intelligence systems may leverage data from previous diagnostic studies to make highly accurate predictions about the mass, to be confirmed by the physician, saving both the patient and the physician valuable time and resources.
Simpler imaging techniques could even be carried out by artificial intelligence medical robots on their own. For example, an ultrasound imaging system could be integrated into an artificial intelligence-assisted robotic arm, enabling complete imaging without the need for a physician.
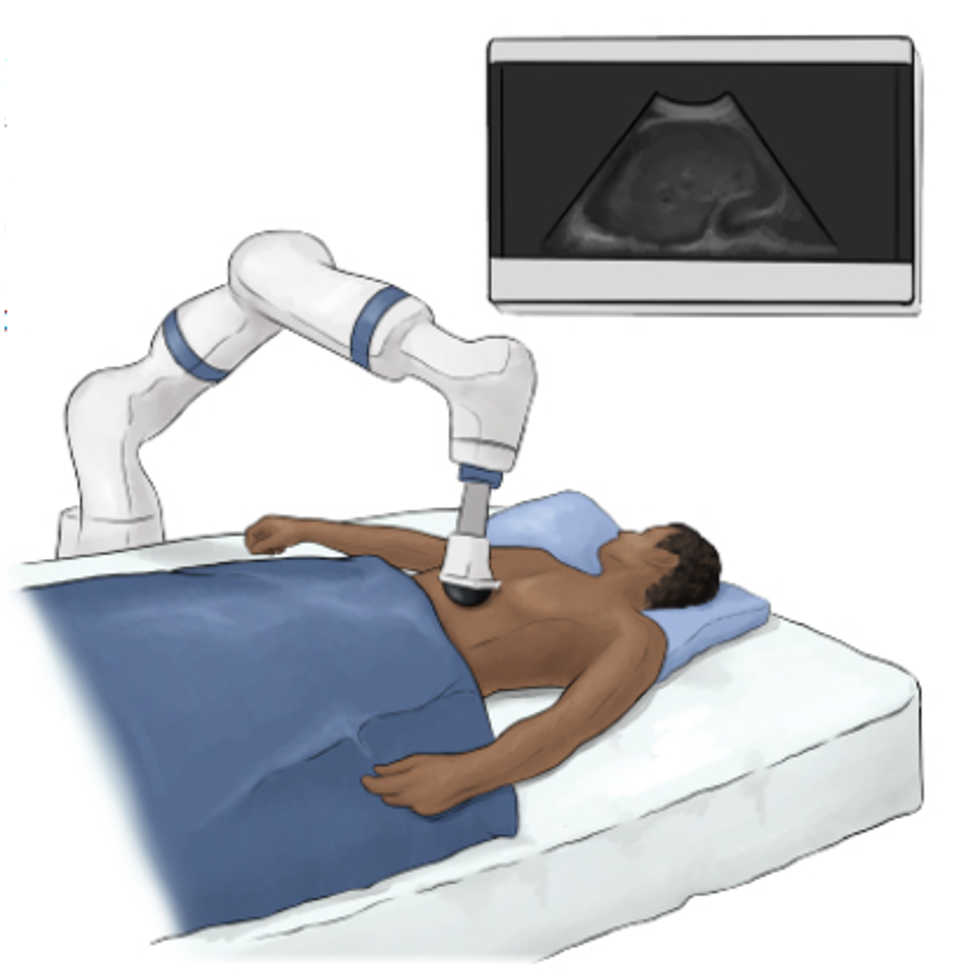
FIGURE 1: Schematic of an AI-assisted ultrasound imaging robot.
For use in surgery, automated artificial intelligence medical robots are few and far between. One such example is the Smart Tissue Autonomous Robot, which can administer sutures without the aid of an operator. Most of these systems are used by physicians as aids for more difficult or intricate surgeries. For example, the Da Vinci robot teleoperation allows physicians to conduct complex procedures by operating robot arms remotely. The artificial intelligence aspect of these devices is the detection and removal of involuntary hand movements, which reduces the risk of tissue damage.
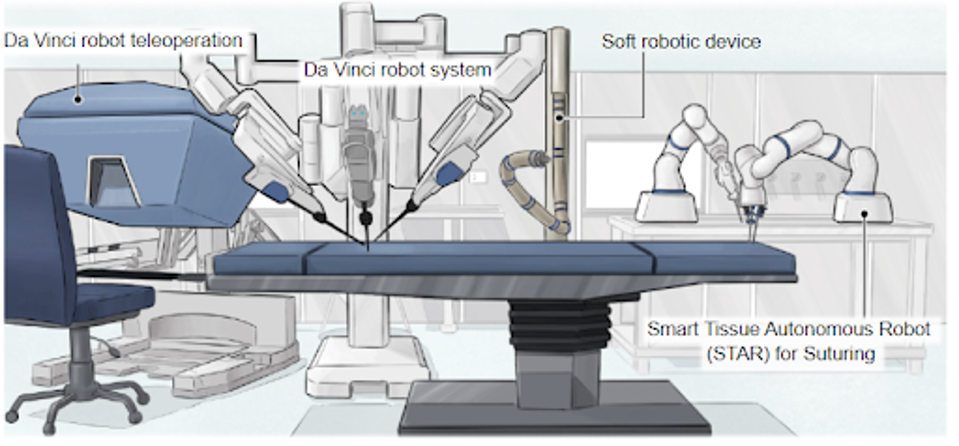
FIGURE 2: Differing types of artificial intelligence-assisted medical robots.
A third common conjunction of artificial intelligence and medical robotics is rehabilitation and advanced prosthetics. I have written extensively on the evolving field of smart robotics in regenerative medicine, which can be found on my website, linked at the end of this article. One such example is that of a neural implant and headset combination that aims to restore sight to the blind by artificially activating photoreceptors in the visual cortex of the brain. All forms of artificial intelligence that could improve rehabilitative practices are welcome additions to the field.
There are, however, a number of challenges to implementing artificial intelligence-assisted robotics in healthcare.
One such challenge is the lack of high-quality medical data. Just as a large language model of artificial intelligence uses massive amounts of data pulled from search engines, medical artificial intelligence systems would require massive amounts of quality health data to determine correct courses of action for actions such as surgery, diagnostics, and diagnoses.
Ongoing issues such as paper records, fragmented medical histories, and poor data management create barriers for artificial intelligence-assisted robotics to excel.
Another set of challenges is reliability and transparency. As these models are often excessively complex, the average patient is unlikely to understand how they operate and may question the validity of the model’s findings. As such, nearly all artificial intelligence-assisted medical robots will likely be assisted by physicians throughout the process, at least for the time being.
A third issue will be the training and cost required to implement these systems. Not only do the systems themselves yield high costs to be implemented, but all healthcare workers will need to be trained to use and understand these systems, which is not often taught in medical school today.
As such, widespread use of these technologies is still years away, but they will arrive. When they do, we must be prepared to have artificial intelligence-assisted robotics as a part of our healthcare system, for better or for worse, as the technology continues to progress.
To read more of this series, please visit www.williamhaseltine.com