 Infant Receiving Oral Polio Vaccine GETTY IMAGES
Infant Receiving Oral Polio Vaccine GETTY IMAGES
This is Part III in a series on the enteroviruses that appear to cause a polio-like neurological disease, Acute Flaccid Myelitis. Hopefully we can use what we have learned from both the success and challenges of poliovirus vaccines to mount a formidable defense against emerging enteroviruses such as those causing Acute Flaccid Myelitis.
Poliomyelitis, more commonly known as polio, has nearly been eradicated worldwide. This is mostly thanks to effective vaccines and the expansive vaccination efforts reaching virtually all ends of the world. Afghanistan and Pakistan are now the only countries left in the world where polio is endemic. However, there have already been multiple cases of paralysis due to polio reported across the globe this year, from Malawi to Ukraine, and poliovirus was very recently detected in wastewater in London. These outbreaks are evidence that the two polio vaccines currently in use are not sufficient to reach complete eradication, and the development of an even safer and more effective vaccine is essential.
Despite the overarching success of vaccination against poliovirus, the push for complete eradication has faced considerable setbacks, with some recent discouraging ones. The entire continent of Africa was declared free of the wild poliovirus in 2020, but at least two new cases were reported in Malawi and Mozambique this year. They were discovered in young children who were both paralyzed as a result of the infection, meaning there are likely other unidentified cases as well. In 95% of cases, the poliovirus is only present in the bloodstream and the infection is asymptomatic. In 5% of cases, the virus spreads and replicates in other areas of the body outside of the bloodstream. The continued viral replication causes sustained secondary viremia and leads to the development of mild symptoms such as fever, headache, and sore throat.
Paralytic poliomyelitis, causing the paralysis polio is infamously known for, occurs in less than 1% of all poliovirus infections. This happens when the virus spreads into the central nervous system and replicates in motor neurons, leading to the selective destruction of said motor neurons in the spinal cord, brain stem, or motor cortex and resulting in temporary or permanent paralysis. We still do not really understand why the virus has very severe effects on some people but spares most others, and the frequency of asymptomatic cases means that there is a high likelihood of additional unidentified resurgent polio cases.
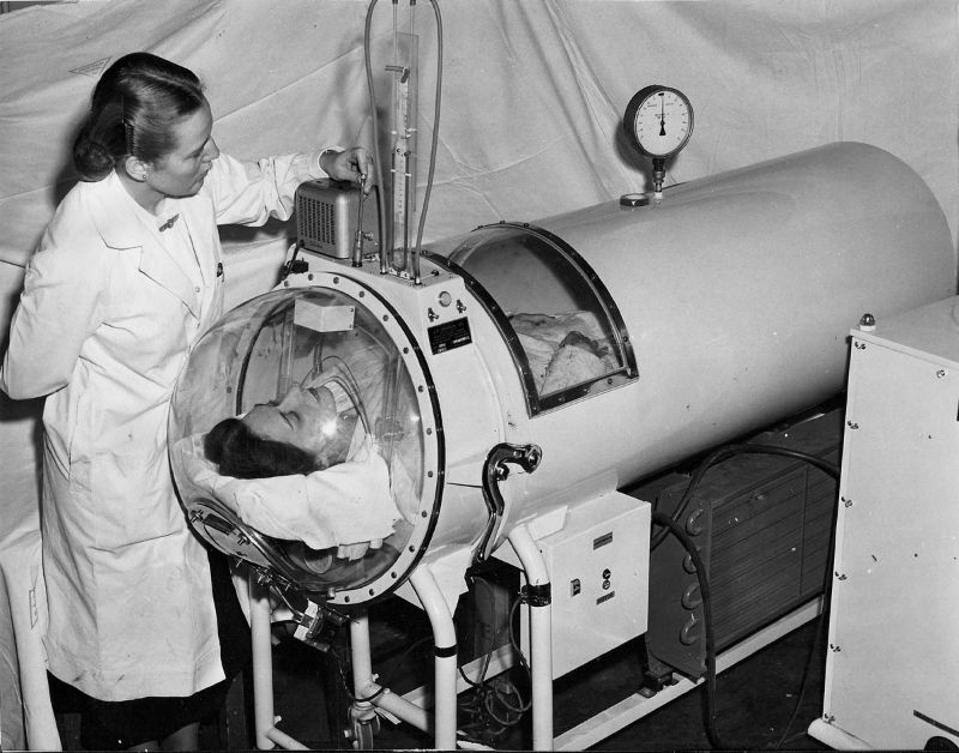 Nurse Checks on Polio Patient in Iron Lung- Photograph from 1940 VINTAGE EVERYDAY
Nurse Checks on Polio Patient in Iron Lung- Photograph from 1940 VINTAGE EVERYDAY
There are two types of poliovirus vaccines that have been in use for decades. One is inactivated, or killed, and given by injection, and the other is live but attenuated, or weakened, and given by mouth. They each have their own set of advantages and disadvantages. The inactivated vaccine was developed in the 1950s, and it has proven to be very safe and effective. Because the virus is killed, there is no chance of mutation causing a reversion to the original pathogenic form and causing disease. However, the protection it provides is only capable of preventing the individual from developing severe disease or paralysis, it does not prevent infection or transmission.
The oral attenuated vaccine, on the other hand, is capable of preventing transmission as well as disease. Developed in the 1960s, the live virus vaccine was essential in curbing the polio pandemic by preventing further spread. Despite this, it is not the perfect solution. The principal complication has been the worldwide emergence of cases of circulating vaccine-derived poliovirus (cVDPV) from the oral poliovirus vaccine. Although this vaccine has been modified to limit pathogenicity, it has the ability to mutate, reverting to a pathogenic form capable of causing severe disease and paralysis. The infection can then spread to and between people who have been vaccinated with the inactivated version of the vaccine.
Although incidence of cVDPV is rare, the recent increase in cases as a result of mutation in the live attenuated virus is cause for concern. In 2021, there were 614 reported cases of cVDPV, largely in Africa and the Middle East. Furthermore, cVDPV can spread just as easily as the wild type, and communities with low vaccination rates and waning immunity are especially susceptible. This includes countries experiencing political conflict such as Yemen and now Ukraine, where weakened healthcare systems mean that children are missing routine vaccinations and national reporting networks are operating at limited capacity.
Due to the clear need for a new and improved vaccine option, there is a novel live oral polio vaccine in development, termed nOPV2. It is very similar to the original live attenuated vaccine, but with some changes that greatly improve genetic stability, meaning mutations leading to reversion to a pathogenic form are much less likely. Under direction of the World Health Organization’s Emergency Use Listing procedure, the Global Polio Eradication Initiative has begun dispersal of the vaccine. While we are still in the early stages of mass administration, nOPV2 is a promising solution to the recent resurgence.
It is estimated that there would be 16 million people paralyzed today by polio if not for vaccination, not to mention countless lives lost. If the goal of worldwide eradication of poliovirus is successful, it will be only the second human infectious disease ever fully eradicated, with smallpox being the first. The new attenuated oral vaccine with further safeguarding against mutation means this future is still in sight. Hopefully, the strategies behind vaccine development and dispersal against polio can aid in the fight against newly emerging enteroviruses from the same family.


