This is the first of two stories describing recent progress in understanding the cause and potential treatment for osteoarthritis. In part two, we will discuss how this discovery may yield clinical benefits. This story is part of an extensive series on regenerative medicine. We define regenerative medicine as any medical modality which restores normal function—whether damaged by disease, injured by trauma, disadvantaged by birth or worn by time. For more on this topic, visit www.williamhaseltine.com and search regenerative medicine.
Osteoarthritis is a joint condition which plagues more than 32.5 million people in the United States—around 1 in every 7 American adults. It is a leading cause of disability, costing the US more than $185 annually. Regrettably, the detailed disease process and treatment are elusive. Here, we describe a recent study published in Science Advances which investigates a possible cause: the inflammatory environment of the joints. In the following story, we will describe how these findings may bring us one step closer to a cure.
What is Osteoarthritis?
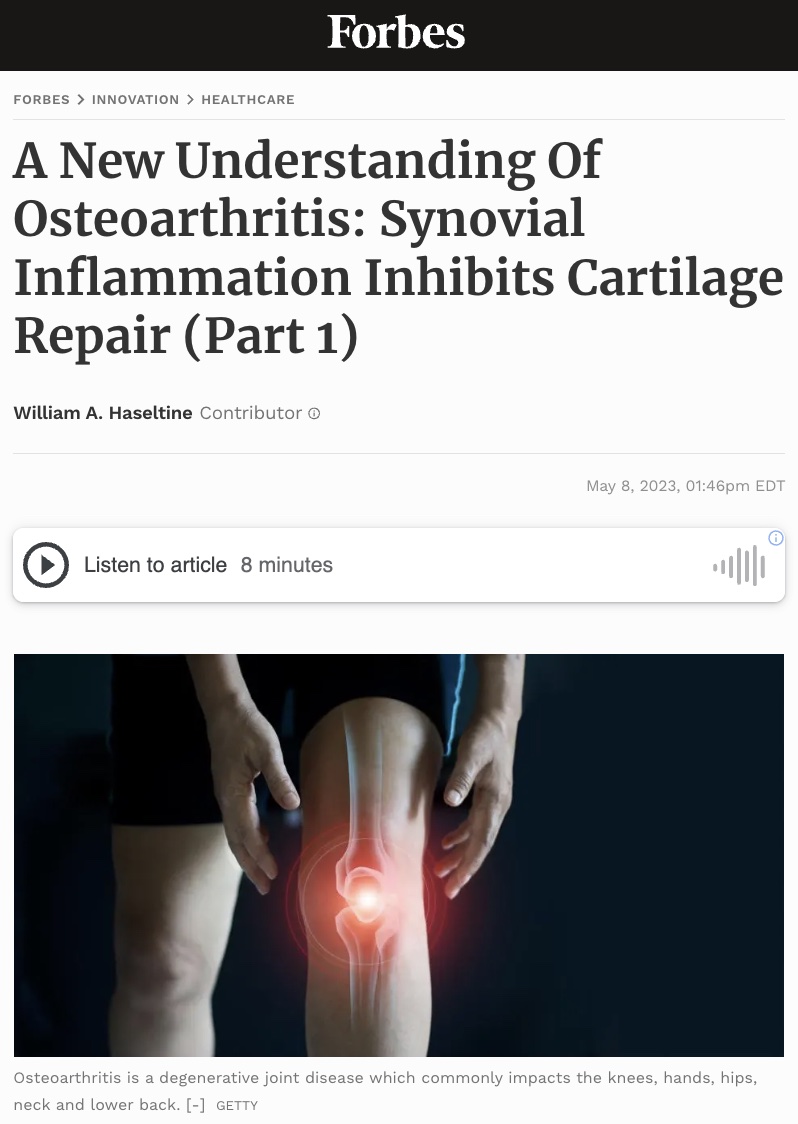
Osteoarthritis is a common form of arthritis characterized by cartilage degeneration. It occurs most frequently in the hands, knees and hips, but any joint can be affected.
Cartilage provides essential padding between any two bone ends. If this cartilage wears away, the joint becomes inflamed and painful. In osteoarthritis, usually the cartilage thins in response to aging or joint injury (Figure 1). The chronic pain, limited movement and reduced function hamper quality of life and can eventually lead to disability. Current treatment regimens are lacking, as they only address symptoms and not the cause.
Several factors play a part in osteoarthritis: a history of joint injury, age, gender, weight, genetics. Importantly, we do not know the precise details of cartilage degeneration.
Figure 1: Comparison of a healthy joint and a joint with osteoarthritis. Osteoarthritis occurs when the cartilage breaks down, causing the bone ends to painfully rub against each other.
HEALTH DIRECT, ELANABSL
Tissue Regeneration and Osteoarthritis
Bolander et al. at the Wake Forest Institute of Regenerative Medicine examined cartilage deterioration in patients with osteoarthritis. Through a series of experiments, they discovered that inflammation in the synovial fluid may be the proximate cause.
Inflammation: The Root Cause of Osteoarthritis
When the joints are injured, as with osteoarthritis, the tissue will attempt to heal the damage. Inflammation naturally accompanies the healing process. However, persistent inflammation prevents proper tissue regeneration and instead results in fibrosis, the accumulation of connective tissue. This failed tissue regeneration is key to osteoarthritis.
Honing in on the Synovial Fluid
The synovial membrane encapsulates the joint, creating a fluid-filled sac. Observations of mice with cartilage damage revealed that the synovial membrane thickened after the injury; this released a flood of progenitor cells, or cells which eventually create new cartilage. A hypothesis formed: if the membrane can successfully initiate the regeneration process, perhaps there are unknown factors in the synovial fluid that may interfere with the healing process.
Capable Joint Cells
Bolander et al. first collected synovial fluid from osteoarthritis patients, and then separated the cells from the fluid. They monitored the cells for three factors of tissue regeneration: the ability to migrate to the injury site, to attach to a tissue surface, and to proliferate. Despite being derived from arthritic synovial fluid, the extracted cells functioned best in all accounts when not in the presence of the diseased fluid.
The cells traveled successfully in the presence of an attractant; in contrast, cell migration decreased significantly when surrounded by synovial fluid. During a 72 hour observation period, the joint cells did not attach to the tissue culture surface whatsoever when in the presence of 100% or 50% of synovial fluid. The proliferation tests performed similarly. The cells were labeled, exposed to either 10% synovial fluid or no synovial fluid, and then monitored for two weeks. The cells exposed to synovial fluid struggled to proliferate in comparison to the control group.
As the results demonstrate, the cells in arthritic joints have an intrinsic ability to heal damaged cartilage. However, these essential processes do not occur when exposed to the same synovial fluid from which they were extracted.
Synovial Fluid Inhibits Differentiation
The next stage of the study involved arthritic progenitor cells. Progenitor cells are crucial to tissue regeneration. Although initially unspecialized, they differentiate into cartilage cells to form a new tissue matrix.
Exposing arthritic cells to arthritic synovial fluid delayed their ability to cluster and form a tissue matrix. What formed, instead, seemed to resemble fibrosis—a failed sign of regeneration. Collagen staining confirmed that the synovial fluid impaired proper collagen production and distribution.
Gene analyses suggested that the synovial fluid of patients with osteoarthritis may inhibit key transcription events needed for cartilage formation. Most notably, there was a major reduction in healthy transcription factors. Examples include a key transcription factor for cartilage formation (box transcription factor 9, SOX9) and a protein which lubricates the joint (proteoglycan 4, PRG4).
Dedifferentiation Markers
The arthritic progenitor cells failed to differentiate in the synovial fluid, but was this a phenomenon that occurred only in this environment? To find out, healthy cartilage cells were placed in the presence and absence of arthritic synovial fluid.
Even though these cells did not come from osteoarthritis patients, they behaved similarly in the synovial environment. The fluid-exposed cells produced fibrotic formations in the three dimensional models, while the controls did not. The subsequent mRNA transcript analysis also showed an increased expression of dedifferentiation markers such as COLL10A in synovial fluid samples. The impaired function of arthritic cells and healthy cells in diseased fluid suggests the synovial fluid as the main culprit.
Proinflammatory Factors in Synovial fluid
Clearly, the synovial fluid contains factors that prevent healthy tissue formation. A protein and cytokine analysis hinted at what exactly those factors may be. The synovial fluid in osteoarthritis patients revealed lower concentrations of pro-regenerative markers (ie, IL-2 and IL-4) and higher concentrations of pro-inflammatory markers (ie. IL-17A, IL-6, IL-10 ) than that of healthy donors.
Bolander and colleagues also isolated two white blood cell groups, macrophages and neutrophils, from healthy donors. These cells, when exposed to osteoarthritic synovial fluid, demonstrated increased migration and proliferation—events which occur during inflammation. Ultimately, the synovial fluid environment contains many inflammation factors which likely contribute to fibrosis.
Implications
The findings of Bolander et al. point to a remarkable discovery. The cells in the joints possess an innate ability to repair tissue damage, but are inhibited by inflammatory factors present in the synovial fluid. This observation has profound implications for treatment development. If the inflammatory fluid environment can be altered, the cells, in theory, would be able to regenerate and restore joint function. In the following installation, we will describe how the authors use these findings to outline a hopeful path for novel osteoarthritis treatments.