All organs in the body rely on the blood and oxygen circulated by the heart. If the muscles of the heart weaken or stiffen too much, the heart—although still beating—can no longer pump enough to sustain other organs. This progressive condition called heart failure presently affects more than 6 million adults in the United States. Current treatments can delay but not permanently alter the course of the disease, leaving many patients with poor prognoses. A recent study published in the Journal of the American College of Cardiology searches for a permanent solution to repair the heart via stem cell therapy.
What are Mesenchymal Stem Cells?
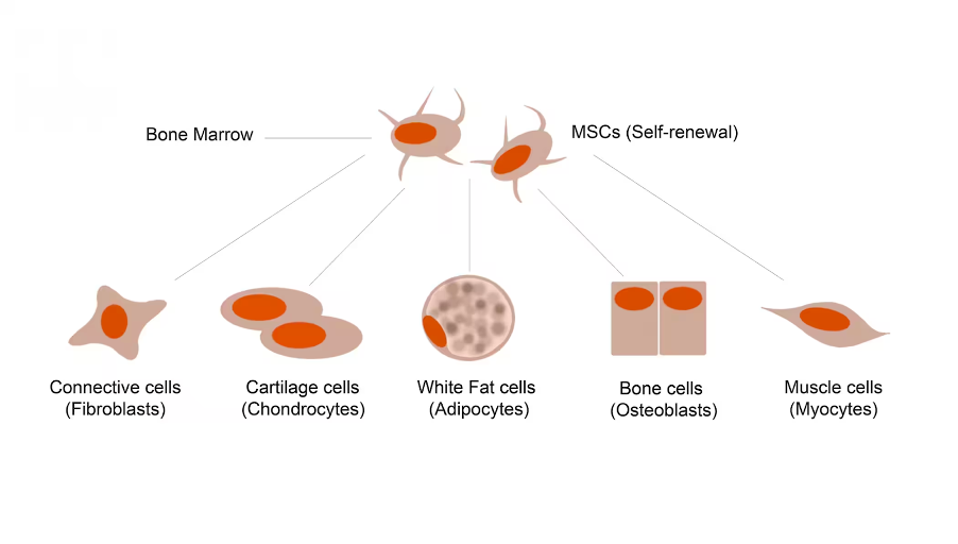
Mesenchymal precursor cells (MPCs) refer to a small population of adult stem cells found in the bone marrow and select tissues. While embryonic stem cells can develop into any cell type in the body, mesenchymal stem cells develop into a defined variety of specialized cells. As Figure 1 illustrates, differentiation of these cells can create connective tissue cells, cartilage cells, white fat cells, bone cells and muscle cells. The ability to regenerate muscle cells is of notable interest in discussions around healing damaged hearts.
FIGURE 1: Mesenchymal stem cells (MSCs) are multipotent adult stem cells; this means that they develop into a certain variety of cells with specific functions (ex: muscle cells).
MILLIPORESIGMA
Mesenchymal precursor cells demonstrate other unique abilities. Preclinical studies suggest that these precursor cells may reduce inflammation driven by macrophages, immune cells involved in the body’s healing processes, and chemicals called cytokines. These stem cells also release proteins which promote the growth of new blood vessels and reverse the narrowing of arteries. These two characteristics may address critical mechanisms which contribute to heart failure: acute and chronic inflammation alongside restricted blood flow to the heart’s tissues.
Clinical Trial Design
For their study, Perin et al. assessed the efficacy of mesenchymal precursor cell therapy on over 500 patients with moderate to severe heart failure. To do this, they first crafted their stem cell product. The researchers derived the stem cells from the bone marrow of three healthy adult donors. They then isolated and proliferated the stem cells before preserving them in liquid nitrogen.
Of all the heart’s chambers, the team focused on the left ventricle. Figure 2 highlights the structure. This section of the heart provides the most pumping power and often falters first for people with heart failure. Left ventricular performance is therefore an important marker of the heart’s condition.
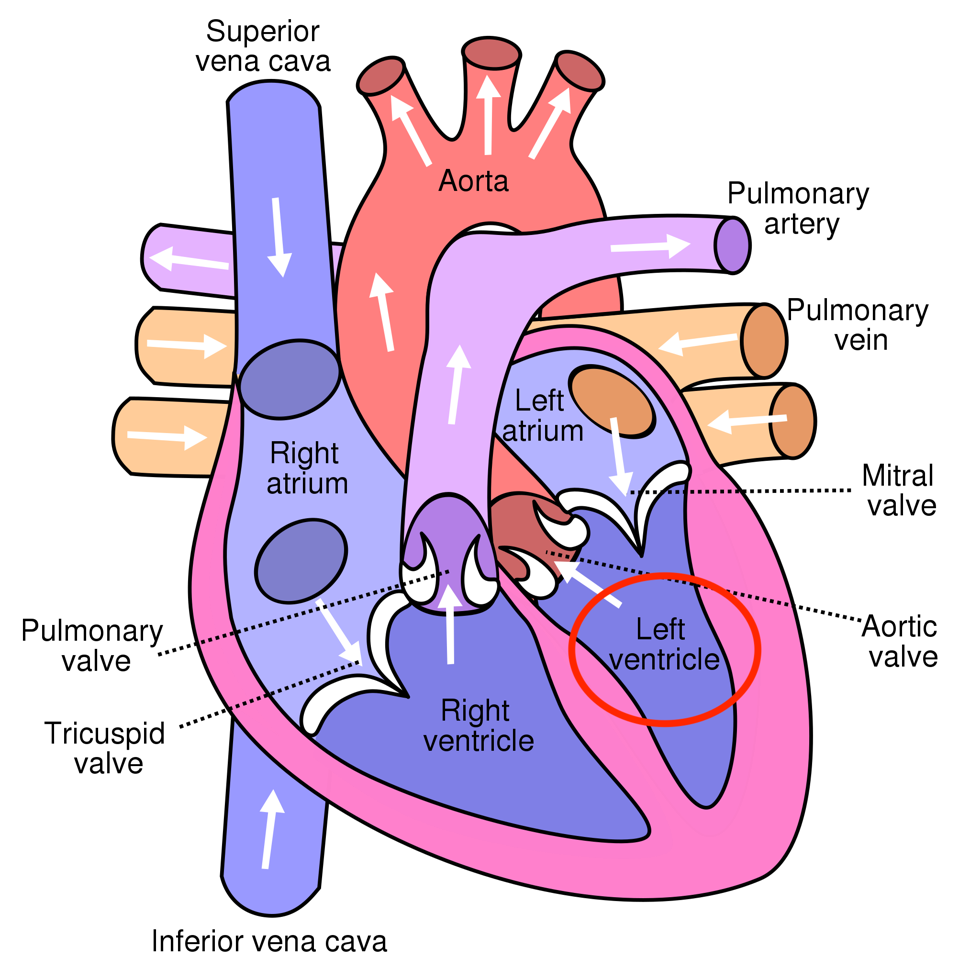
FIGURE 2: Diagram of the heart. Heart failure results when the heart weakens or stiffens so much that it becomes difficult to support the other organs in the body. It is important to recognize the left ventricle (in red) for this study. This chamber of the heart has the most pumping power and is often the first chamber to weaken in heart failure.
WIKIPEDIA
Half of the study population received at least one dose of the cell therapy injection (see Figure 3) into the left ventricle. In contrast, the other half—the control group—underwent a procedure to remove a catheter from the left ventricle. The researchers then conducted site follow-ups 10 days after and on months 1, 3, 6 and 12. After month 12, the patients returned to the site every six months. The team followed the patients for around 30 months on average.
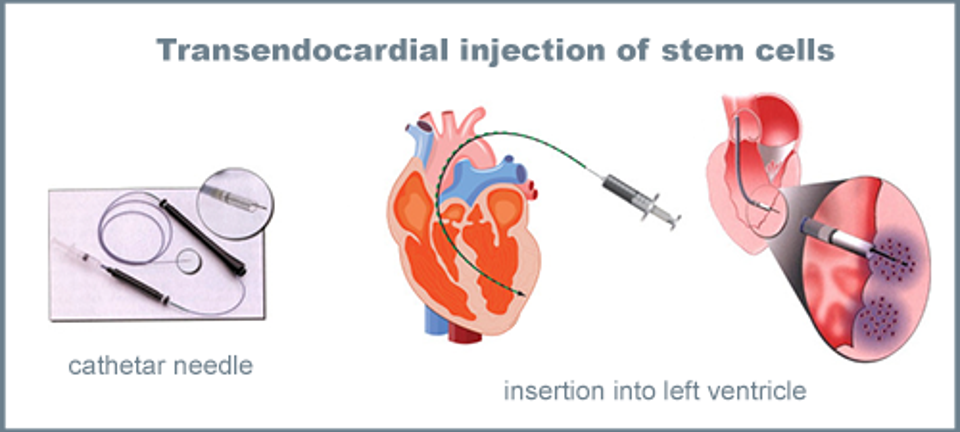
FIGURE 3: The researchers used a catheter (left) to administer the stem cell therapy. A transendocardial injection involves inserting the catheter into the heart through the aortic valve into the left ventricle. There, the needle injects the stem cells into the endocardial surface (right).
E.C PERIN, 2018; PARAJULI AND DONAHUE, 2020.
Study Endpoints and Measurements
The study contained two main objectives to understand the potential benefits of the intervention. The primary endpoint measured whether the therapy prolonged the time to a patient’s next nonfatal hospitalization or urgent care visit; it was considered a terminal event if a patient’s left ventricle failed to provide the majority or any of the heart’s output. The secondary measurement recorded both the primary endpoint and the time to death.
Guided by a previous study, the team monitored left ventricular function and markers of inflammation for additional analysis. Left ventricular performance plays a major role in determining heart failure, while high baseline levels of high-sensitivity C-reactive protein (hsCRP)—a marker of inflammation—in patient plasma is associated with adverse cardiac events.
Mixed Results
The clinical trial yielded mixed results. The team found no significant difference between the treatment groups for the study’s primary and secondary endpoints, suggesting that the therapy did not succeed. However, the therapy produced major findings related to heart function which hold great promise for future research.
Inflammation, Heart Attack and Non Fatal Stroke
The team noticed that adverse heart events could be stratified by inflammation. A single stem cell injection resulted in a 67% reduction in heart attack and a 56% reduction in stroke compared to controls. Figure 4 illustrates the clear difference in risk. Interestingly, the supposed benefit increased if the patient displayed higher levels of inflammation (see Figure 5).
Additionally, the therapy led to a modest reduction—38% specifically—in three point major adverse cardiovascular events. This is categorized by a cardiovascular death, nonfatal heart attack or nonfatal stroke. Patients with more detectable inflammation saw a larger effect here, as well.
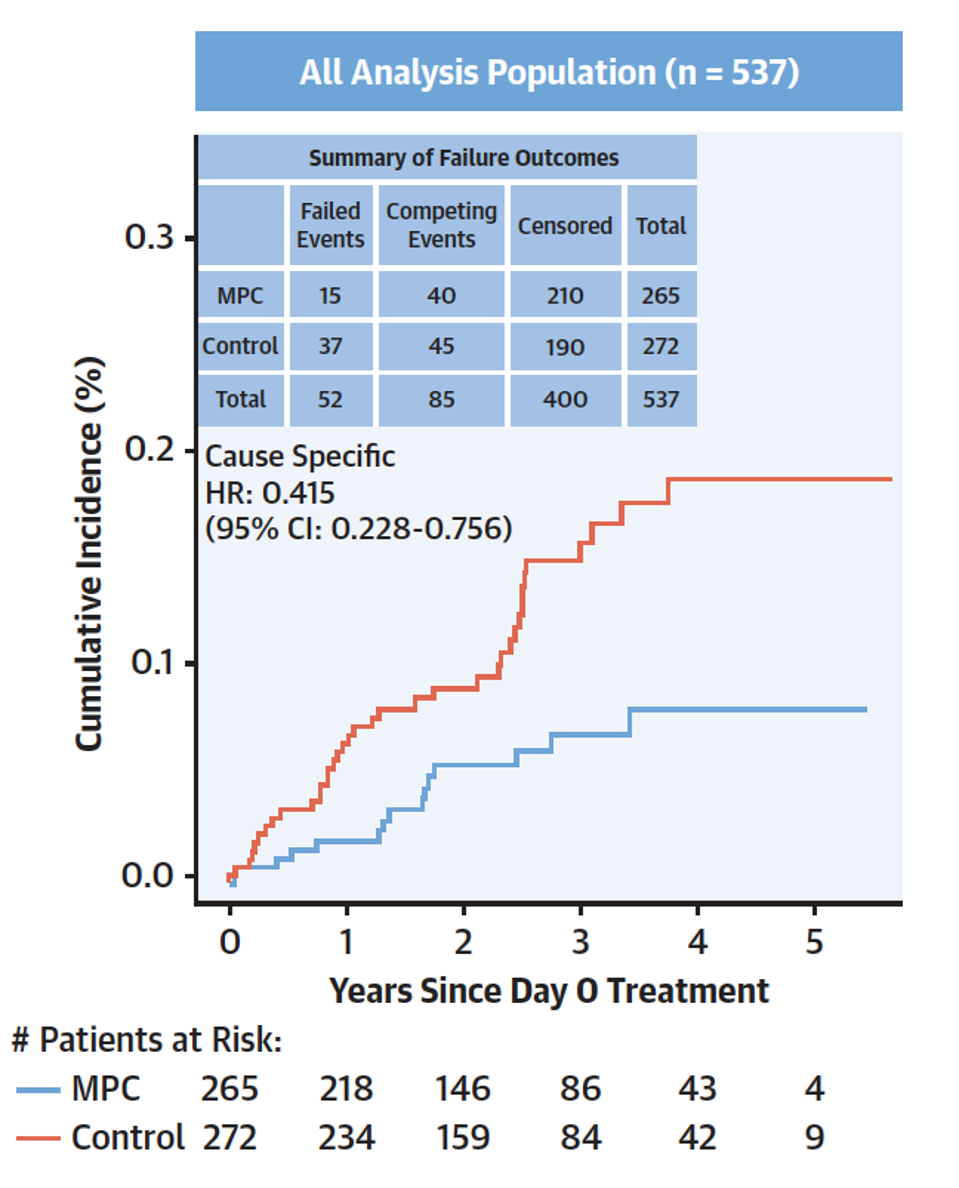
FIGURE 4: Heart failure patients (blue) who received the cell therapy displayed a large reduction in either heart attack or stroke compared to patient controls (red). Abbreviations: MPC, mesenchymal precursor cells; HR, hazard ratio; CI, confidence interval.
PERIN ET AL, 2023.
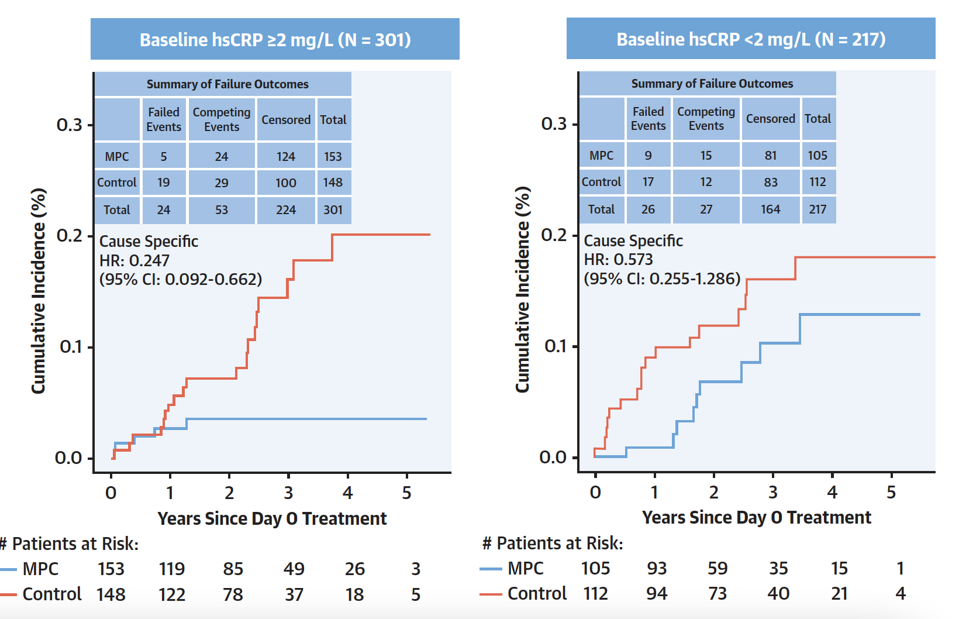
FIGURE 5: Comparison of heart attack or stroke reduction by inflammation level. Patients with a higher inflammation level (left) demonstrated a greater reduction than patients with lower baseline inflammation (right). Abbreviations: hsCRP, high-sensitivity C-reactive protein (a marker of inflammation).
PERIN ET AL, 2023.
Inflammation and the Left Ventricle
The team used echocardiographic imaging to glean information about the left ventricle. They recorded three measurements in particular: left ventricular ejection fraction (LVEF), or how much blood the left ventricle pumps out during each heartbeat; left ventricular end-systolic volume (LVESV), or how blood remains in the chamber after a heartbeat; and left ventricular end diastolic volume (LVEDV), how much blood is in the chamber before a heart beat.
The patients who received the cell therapy experienced a small but statistically significant improvement in their heart’s ability to pump over the course of a year. This is mostly attributed to the effect experienced by patients with higher levels of inflammation. In comparison, the therapy did not influence the left ventricular diastolic volume when compared to controls.
Possible Mechanisms
The clinical hope for cell therapy is to harness the self-renewing and tissue regenerating capabilities of stem cells to heal and repair the body. The mesenchymal stem cells injection in this study did not meet this goal; the therapy failed to reduce time to nonfatal hospitalization and all cause death for patients with heart failure. However, an interesting discovery did emerge regarding inflammation.
The stem cell therapy created by Perin et al. yielded larger perceived benefits for patients with higher detectable levels of inflammation. Heart attack, stroke and left ventricular function appeared to improve for patients with evidence of systemic inflammation. How could this difference be explained?
Background research suggests that targeting inflammation could reduce negative heart events. Animal studies of heart failure demonstrated how mesenchymal precursor cells could rebuild and generate new blood vessels; they, too, could reverse the narrowing of arteries throughout the heart and body in the presence of systemic inflammation. The authors posit, then, that their cell therapy may alter inflammatory environments in the heart and promote blood flow through the formation of new blood vessels.
The cytokines found around the heart may activate the mesenchymal cells, causing the stem cells to subsequently release proteins which suppress inflammation and encourage blood vessel formation. The anti-inflammatory effects likely reduce nonfatal heart attack, stroke and death for patients with high inflammation. On the other hand, the new blood vessels likely improve the function of the left ventricle, as noted in the study.
As the stem cells appear to target local and systemic inflammatory changes seen in heart failure and atherosclerosis (plaque-filled arteries), Perin et al. turn to inflammation as a possible therapeutic target for heart failure. The therapy, when used in conjunction with existing heart failure treatments, may provide additional clinical benefit to patients with increased inflammation.
Future Implications
This clinical trial marks an important step in the journey to use cell therapy to reverse heart failure. Although the therapy did not prevent hospitalization as initially hoped, the researchers found that a single stem cell injection reduced the risk of heart attack or stroke by more than 50% for people with heart failure. Stem cell therapy may be a complementary addition to heart failure treatment regimes in the future, but further research is needed to ascertain its promise.