Organoids offer new insight into the effects of Covid-19 infection on pregnant women and their children. In a recent study, Australian researchers led by Dr. Jose Polo from Monash University, develop a placental organoid model that demonstrates how the SARS-CoV-2 virus infects the placental barrier between maternal and fetal blood, impairing the barrier’s ability to function.
The study sheds light on why unvaccinated, pregnant women infected with SARS-CoV-2 exhibit an increased risk of having stillborn or preterm infants. It also offers an explanation for why the risk of developing severe disease from viral infections is more likely in pregnant women than in non-pregnant women.
To investigate the effects of SARS-CoV-2 on pregnant women and their children, the research team grew placental organoids. Organoids are created from stem cells. Stem cells have the remarkable ability to develop into almost any cell type. When these cells are provided with the correct environmental and chemical cues, they can be coaxed into interacting with each other and forming human tissue, including tissue that makes up structures like the placenta.
The research team created their placental organoid using human skin cells. By exposing the human skin cells to specific chemical cues, the team reprogrammed the skin cells into trophoblast stem cells. Trophoblast stem cells can ultimately develop into two different types of placental cells—extravillous cytotrophoblasts and syncytiotrophoblasts.
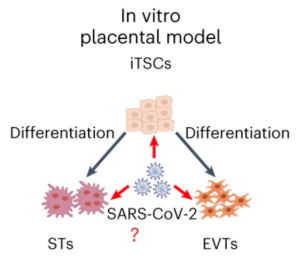
Figure 1: The paper relied on using trophoblast stem cells (iTSCs) to form placental cells like syncytiotrophoblasts (STs) and extravillous cytotrophoblasts (EVTs).
CHEN ET AL., NATURE CELL BIOLOGY (2023), DOI: 10.1038/S41556-023-01182-0
After culturing the placental cells and producing the organoid, the researchers examined the lab-grown placental tissue for any receptors that are traditionally involved in SARS-CoV-2 infection. Two factors that are important for SARS-CoV-2 infection are ACE2 and transmembrane serine protease 2.
ACE2 is a receptor protein that provides an entry point for SARS-CoV-2 infection. Transmembrane serine protease 2 activates the SARS-CoV-2 viral spike protein and improves the virus’s ability to enter cells through the ACE2 receptor. By staining the lab-grown placental tissue, the researchers confirmed that the tissue expressed both ACE2 and TMPRSS2. These proteins were especially expressed in syncytiotrophoblasts.
Next, the team infected their placental tissue with the SARS-CoV-2 virus. Interestingly, while the virus easily infected syncytiotrophoblast cells, the trophoblast stem cells and extravillous cytotrophoblasts remained uninfected. These results were also consistent when the researchers infected the cells with the Delta and Omicron variants of SARS-CoV-2.
As the syncytiotrophoblasts were the only cells infected by SARS-CoV-2, the researchers focused on assessing how the infection impaired syncytiotrophoblast function. The syncytiotrophoblast is a layer of the placenta that contains a spectrum of cells ranging from immature stem cells to fully developed syncytial cells. The placental layer plays a crucial role in nutrient and gas exchange between the mother and infant.
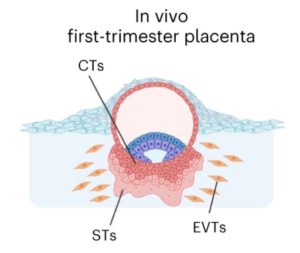
Figure 2: Researchers focused their efforts on syncytiotrophoblast cells (STs) which form a crucial layer of the human placenta.
CHEN ET AL., NATURE CELL BIOLOGY (2023), DOI: 10.1038/S41556-023-01182-0
After analyzing the syncytiotrophoblast cells, researchers found that the infected cells were less mature than non-infected cells. Similarly, they observed that the infected tissue contained a higher proportion of immature stem cells. These results suggest that SARS-CoV-2 infection reduces the growth and development of syncytiotrophoblast tissue.
Another measure of cell function is the level of cytotoxic stress. Cytotoxic stress occurs when external influences cause cell damage or death. To examine whether SARS-CoV-2 increases cytotoxic stress, the researchers tested their samples for chemicals that cells release when they are damaged. As expected, the infected cells released significantly higher levels of damage-induced signals.
To develop a deeper understanding of the effects of SARS-CoV-2 infection on the syncytiotrophoblast cells, researchers then ran genetic tests on the cells. The results of the genetic tests determined that the infected cells expressed genes differently than the non-infected ones. Importantly, genes that were specific to the function of syncytiotrophoblasts were expressed significantly less than the uninfected cells. This pointed to a loss of function in the syncytiotrophoblasts after infection with SARS-CoV-2.
These results led to an important question; how could the researchers prevent SARS-CoV-2 infection in syncytiotrophoblasts?
Since ACE2 serves as an entry point for the virus, the researchers investigated whether the ACE2 receptor could be targeted to inhibit the virus from entering the cell. To do so, they created an anti-ACE2 antibody that could potentially block viral entry.
To test their anti-ACE2 antibody, the researchers exposed the cells to the antibody and the virus, then assessed whether the cells were infected with the virus. To their surprise, the researchers did not detect the infectious virus in cells treated with the anti-ACE2 antibody. Additionally, the cells treated with the anti-ACE2 antibody displayed similar gene expression as healthy, uninfected cells. These results demonstrate that an anti-ACE2 antibody can effectively protect syncytiotrophoblast cells against SARS-CoV-2 infection.
Overall, this study provides valuable insight into how viruses like SARS-CoV-2 affect not only pregnant women but their unborn infants. While more research must be done to understand whether anti-ACE2 antibodies can completely prevent infections in human subjects, these results mark significant progress towards treatments that could provide greater viral protection for pregnant women and their children.